Radiomics: A step towards precision medicine
A key goal of modern medicine is "precision medicine", the purpose of which is to personalise treatment based on the patient’s specific characteristics of the disease. Radiomics is rapidly emerging as a personalised medicine technology and is currently one of the most interesting fields of research.
To understand what Radiomics is, it is necessary to start by saying that some tumours are characterised by molecular alterations, such as genomic alterations. Given that it is possible to define these alterations, it is generally necessary to have a sample of the neoplastic tissue, which is obtained by biopsies or invasive surgical interventions. Currently, however, imaging diagnostics can enable tissues to be characterised in a non-invasive manner and, in some cases, can enable the profound phenotypic differences to be visualised. Since tumours are heterogeneous in their volume and change over time, diagnostic images can provide a full view of the entire tumour and can be repeated over time to monitor the changes induced by therapies.
Through Radiomics, the medical images, obtained by CT, MRI or PET scans, are converted into numerical data. They are calculated by calculation tools and their analysis often required the use of advanced techniques, such as artificial intelligence methods.
This huge wealth of numerical data, which could not possibly be processed by means of simple visual observation, defines many characteristics of the tumour and the surrounding environment, related, for example, to its shape, volume and tissue structure.
It is possible to study the relationship between the data obtained from the images and the molecular and genomic characteristics of the tumour, with the final aim of extracting indications - directly from the images - regarding the aggressiveness of the disease, the most indicated therapies and its response to treatment.
Hopefully, in the near future, radiological imaging and radiomic models will be used as a decision-making support to clinical practice, to improve diagnostic accuracy and prognostic power.
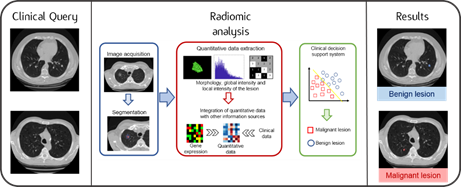
Graphical abstract of the Radiomics workflow: quantitative parameters calculated from clinical images are analysed in combination with the patient’s biological, genetic and clinical characteristics. Thanks to the use of advanced techniques, it is possible to obtain useful information for diagnosis and for personalising treatment.
-
Artificial intelligence (AI) and Radiomic board
The Artificial intelligence (AI) and Radiomic board coordinates Radiomics projects and Medical Imaging based studies proposed by multiple divisions and is responsible for their preliminary assessment, feasibility, management, supervision, support and development.
The Artificial intelligence (AI) and Radiomic board is currently directed by Prof. Roberto Orecchia and is composed by Prof. Massimo Bellomi (Radiology), Dr. Enrico Cassano (Breast Radiology, IEO), Dr. Francesco Ceci (Imaging Diagnostics, IEO), Dr. Marta Cremonesi (Radiation Research, IEO), Prof. Giuseppe Curigliano (New Drugs and Early Drug Development for Innovative Therapies, IEO), Dr. Aurora Gaeta (Biostatisticians, IEO), Prof. Sara Gandini (Biostatisticians, IEO), Prof. Barbara Jereczek (Radiotherapy, IEO), Prof. Davide La Torre (Artificial Intelligence and Mathematical Imaging, University of Milan), Dr. Sofia Netti (Biostatisticians, IEO), Prof. Giuseppe Petralia (Radiology), Dr. Paola Queirolo (Medical Oncology of Melanoma and Sarcomas, IEO), Dr. Cristiano Rampinelli (Radiology, IEO).
The Artificial intelligence (AI) and Radiomic board meets monthly to discuss together new proposals and the progress of ongoing studies. Since February 2022, the meetings, which are held online, include an open session for anyone who is interested.
Open meetings are scheduled every third Thursday of the month, excluding July and August, from 2:30 to 3 p.m.
We look forward to your participation. For more information and to participate, please write to inforadiomica@ieo.it.
-
PUBLICATIONS
- Volpe S, Mastroleo F, Krengli M, et al. Quo vadis Radiomics? Bibliometric analysis of 10-year Radiomics journey. Eur Radiol (2023). https://doi.org/10.1007/s00330-023-09645-6
- Travaini LL, Botta F, Derenzini E et al. [18 F]-FDG PET radiomic model as prognostic biomarker in diffuse large B-cell lymphoma. Hematol Oncol 2023. https://doi.org/ 10.1002/hon.3171
- Volpe S, Gaeta A, Colombo F, et al. Blood- and Imaging-Derived Biomarkers for Oncological Outcome Modelling in Oropharyngeal Cancer: Exploring the Low-Hanging Fruit. Cancers. 2023;15(7):2022. https://doi.org/10.3390/cancers15072022
- Pesapane F, De Marco P, Rapino A, et al. How Radiomics Can Improve Breast Cancer Diagnosis and Treatment. Journal of Clinical Medicine. 2023;12(4):1372. https://doi.org/10.3390/jcm12041372
- Nicosia L, Pesapane F, Bozzini AC, et al. Prediction of the Malignancy of a Breast Lesion Detected on Breast Ultrasound: Radiomics Applied to Clinical Practice. Cancers. 2023;15(3):964. https://doi.org/10.3390/cancers15030964
- Mossinelli C, Tagliabue M, Ruju F, et al. The role of radiomics in tongue cancer: A new tool for prognosis prediction. Head & Neck. 2023;45(4):849-861. https://doi.org/10.1002/hed.27299
- Pesapane F, Rotili A, Valconi E, et al. Women's perceptions attitudes to the use of AI in breast cancer screening: a survey in a cancer referral center. The British Journal of Radiology. 2022;95(1132):20220569. https://doi.org/10.1259/bjr.20220569
- Carloni G, Garibaldi C, Marvaso G, et al. Brain metastases from NSCLC treated with stereotactic radiotherapy: prediction mismatch between two different radiomic platforms. Radiotherapy and Oncology. 2022;178:109424. https://doi.org/10.1016/j.radonc.2022.11.013
- Botta F, Ferrari M, Raimondi S, et al. The Impact of Segmentation Method and Target Lesion Selection on Radiomic Analysis of 18F-FDG PET Images in Diffuse Large B-Cell Lymphoma. Applied Sciences. 2022;12(19):9678. https://doi.org/10.3390/app12199678
- Isaksson LJ, Repetto M, Summers PE, et al. High-performance prediction models for prostate cancer radiomics. Informatics in Medicine Unlocked. 2023;37:101161. https://doi.org/10.1016/j.imu.2023.101161
- Nicosia L, Bozzini AC, Ballerini D, et al. Radiomic Features Applied to Contrast Enhancement Spectral Mammography: Possibility to Predict Breast Cancer Molecular Subtypes in a Non-Invasive Manner. International Journal of Molecular Sciences. 2022;23(23):15322. https://doi.org/10.3390/ijms232315322
- Pesapane F, Agazzi GM, Rotili A, et al. Prediction of the Pathological Response to Neoadjuvant Chemotherapy in Breast Cancer Patients With MRI-Radiomics: A Systematic Review and Meta-analysis. Current Problems in Cancer. 2022;46(5):100883. https://doi.org/10.1016/j.currproblcancer.2022.100883
- Santinha J, Bianchini L, Figueiredo M, et al. Discrimination of Tumor Texture Based on MRI Radiomic Features: Is There a Volume Threshold? A Phantom Study. Applied Sciences. 2022;12(11):5465. https://doi.org/10.3390/app12115465
- Elhalawani H, Volpe S, Barua S, et al. Exploration of an Early Imaging Biomarker of Osteoradionecrosis in Oropharyngeal Cancer Patients: Case-Control Study of the Temporal Changes of Mandibular Radiomics Features. International Journal of Radiation Oncology Biology Physics. 2023;100(5):1363-1364. https://doi.org/10.1016/j.ijrobp.2017.12.146
- Isaksson LJ, Pepa M, Summers P, et al. Comparison of automated segmentation techniques for magnetic resonance images of the prostate. BMC Medical Imaging. 2023;23:32. https://doi.org/10.1186/s12880-023-00974-y
- Volpe S, Isaksson LJ, Zaffaroni M, et al. Impact of image filtering and assessment of volume-confounding effects on CT radiomic features and derived survival models in NSCLC. Translational Lung Cancer Research. 2022;11(12):2452-2463. https://doi.org/10.21037/tlcr-22-248
- Mazzara S, Travaini L, Botta F, et al. Gene expression profiling and FDG-PET radiomics uncover radiometabolic signatures associated with outcome in DLBCL. Blood Advances. 2023;7(4):630-643. https://doi.org/10.1182/bloodadvances.2022007825
- Isaksson LJ, Summers P, Bhalerao A, et al. Quality assurance for automatically generated contours with additional deep learning. Insights into Imaging. 2022;13:137. https://doi.org/10.1186/s13244-022-01276-7
- Garau N, Orro A, Summers P, et al. Integrating Biological and Radiological Data in a Structured Repository: a Data Model Applied to the COSMOS Case Study. Journal of Digital Imaging. 2022;35:970-982. https://doi.org/10.1007/s10278-022-00615-w
- Avesani G, Tran HE, Cammarata G, et al. CT-Based Radiomics and Deep Learning for BRCA Mutation and Progression-Free Survival Prediction in Ovarian Cancer Using a Multicentric Dataset. Cancers. 2022;14(11):2739. https://doi.org/10.3390/cancers14112739
- Zerella MA, Zaffaroni M, Ronci G, et al. Single fraction ablative preoperative radiation treatment for early-stage breast cancer: the CRYSTAL study – a phase I/II clinical trial protocol. BMC Cancer. 2022;22:358. https://doi.org/10.1186/s12885-022-09305-w
- Rinaldi L, Pezzotta F, Santaniello T, et al. HeLLePhant: A phantom mimicking non-small cell lung cancer for texture analysis in CT images. Physica Medica. 2022;97:13-24. https://doi.org/10.1016/j.ejmp.2022.03.010
- Rinaldi L, De Angelis SP, Raimondi S, et al. Reproducibility of radiomic features in CT images of NSCLC patients: an integrative analysis on the impact of acquisition and reconstruction parameters. European Radiology Experimental. 2022;6:2. https://doi.org/10.1186/s41747-021-00258-6
- Alcalay M, Jereczek-Fossa BA, Pepa M, et al. Biomedical omics: first insights of a new MSc degree of the University of Milan. Tumori Journal. 2022;108(1):6-11. https://doi.org/10.1177/03008916211047268
- Isaksson L, Summers P, Raimondi S, et al. Mixup (Sample Pairing) Can Improve the Performance of Deep Segmentation Networks. Journal of Artificial Intelligence and Soft Computing Research. 2022;12(1):29-39. https://doi.org/10.2478/jaiscr-2022-0003
- Gugliandolo SG, Pepa M, Isaksson LJ, et al. MRI-based radiomics signature for localized prostate cancer: a new clinical tool for cancer aggressiveness prediction? Sub-study of prospective phase II trial on ultra-hypofractionated radiotherapy (AIRC IG-13218). European Radiology. 2021;31:716-728. https://doi.org/10.1007/s00330-020-07105-z
- Rinaldi L, De Angelis SP, Raimondi S, et al. Reproducibility of radiomic features in CT images of NSCLC patients: an integrative analysis on the impact of acquisition and reconstruction parameters. European Radiology Experimental. 2022;6:2. https://doi.org/10.1186/s41747-021-00258-6
- Volpe S, Pepa M, Zaffaroni M, Bellerba F, et al. Machine Learning for Head and Neck Cancer: A Safe Bet? - A Clinically Oriented Systematic Review for the Radiation Oncologist. Frontiers in Oncology. 2021;11. https://doi.org/10.3389/fonc.2021.772663
- Garau N, Paganelli C, Summers P, et al. A segmentation tool for pulmonary nodules in lung cancer screening: Testing and clinical usage. Physica Medica. 2021;90:23-29. https://doi.org/10.1016/j.ejmp.2021.08.011
- Pesapane F, Rotili A, Botta F, et al. Radiomics of MRI for the Prediction of the Pathological Response to Neoadjuvant Chemotherapy in Breast Cancer Patients: A Single Referral Centre Analysis. Cancers. 2021;13(17):4271. https://doi.org/10.3390/cancers13174271
- Pesapane F, Rotili A, Agazzi GM, Botta F, et al. Recent Radiomics Advancements in Breast Cancer: Lessons and Pitfalls for the Next Future. Current Oncology. 2021;28(4):2351-2372. https://doi.org/10.3390/curroncol28040217
- Barua S, Elhalawani H, Volpe S, et al. Longitudinal radiomics correlate with osteoradionecrosis. Frontiers in Artificial Intelligence. 2021;4:618469. https://doi.org/10.3389/frai.2021.618469
- Colombo A, Bombelli L, Summers PE, et al. Effects of Sex and Age on Fat Fraction, Diffusion-Weighted Image Signal Intensity and Apparent Diffusion Coefficient in the Bone Marrow of Asymptomatic Individuals: A Cross-Sectional Whole-Body MRI Study. Diagnostics. 2021;11(5):913. https://doi.org/10.3390/diagnostics11050913
- Retico A, Avanzo M, Boccali T, et al. Enhancing the impact of Artificial Intelligence in Medicine: A joint AIFM-INFN Italian initiative for a dedicated cloud-based computing infrastructure. Physica Medica. 2021;91:140-150. https://doi.org/10.1016/j.ejmp.2021.10.005
- Placidi L, Gioscio E, Garibaldi C, et al. Multicentre Evaluation of Dosiomics Features Reproducibility, Stability and Sensitivity. Cancers. 2021;13:3835. https://doi.org/10.3390/cancers13153835
- Corso F, Tini G, Lo Presti G, et al. The Challenge of Choosing the Best Classification Method in Radiomic Analyses: Recommendations and Applications to Lung Cancer CT Images. Cancers. 2021;13:3088. https://doi.org/10.3390/cancers13123088
- Bianchini L, Santinha J, Loução N, et al. A multicenter study on radiomic features from T2-weighted images of a customized MR pelvic phantom setting the basis for robust radiomic models in clinics. Magnetic Resonance in Medicine. 2020;00:1-14. https://doi.org/10.1002/mrm.28521
- Avanzo M, Trianni A, Botta F, et al. Artificial Intelligence and the Medical Physicist: Welcome to the Machine. Applied Sciences. 2021;11:1691. https://doi.org/10.3390/app11041691
- Colombo A, Saia G, Azzena AA, et al. Semi-Automated Segmentation of Bone Metastases from Whole-Body MRI: Reproducibility of Apparent Diffusion Coefficient Measurements. Diagnostics. 2021;11(3):499. https://doi.org/10.3390/diagnostics11030499
- Garau N, Paganelli C, Summers P, et al. External validation of radiomics-based predictive models in low-dose CT screening for early lung cancer diagnosis. Medical Physics. 2020;47:4125-4136. https://doi.org/10.1002/mp.14308
- Giannitto C, Marvaso G, Botta F, et al. Association of quantitative MRI-based radiomic features with prognostic factors and recurrence rate in oropharyngeal squamous cell carcinoma. Neoplasma. 2020;67(6):1437-1446. https://doi.org/10.4149/neo_2020_200310N249
- Botta F, Raimondi S, Rinaldi, et al. Association of a CT-Based Clinical and Radiomics Score of Non-Small Cell Lung Cancer (NSCLC) with Lymph Node Status and Overall Survival. Cancers. 2020;12(6):1432. https://doi.org/10.3390/cancers12061432
- Bianchini L, Botta F, Origgi D, et al. PETER PHAN: An MRI phantom for the optimisation of radiomic studies of the female pelvis. Physica Medica. 2020;71:71-81. https://doi.org/10.1016/j.ejmp.2020.02.003
- Isaksson LJ, Pepa M, Zaffaroni M, et al. Machine learning-based models for prediction of toxicity outcomes in radiotherapy. Frontiers in Oncology. 2020;10:790. https://doi.org/10.3389/fonc.2020.00790
- Isaksson LJ, Raimondi S, Botta F, et al. Effects of MRI image normalization techniques in prostate cancer radiomics. Physica Medica. 2020;71:7-13. https://doi.org/10.1016/j.ejmp.2020.02.007
- Pesapane F, Suter MB, Rotili A, et al. Will traditional biopsy be substituted by radiomics and liquid biopsy for breast cancer diagnosis and characterisation? Medical Oncology. 2020;37(3):29. https://doi.org/10.1007/s12032-020-01353-1
- Savini A, Feliciani G, Amadori M, et al. The Role of Acquisition Angle in Digital Breast Tomosynthesis: A Texture Analysis Study. Applied Sciences. 2020;10:6047. https://doi.org/10.3390/app10176047
- Sarnelli A, Mezzenga E, Vagheggini A, et al. Texture analysis in 177Lu SPECT phantom images: Statistical assessment of uniformity requirements using texture features. PLOS ONE. 2019;14(7):e0218814. https://doi.org/10.1371/journal.pone.0218814
- Rizzo S, Raimondi S, de Jong EEC, et al. Genomics of non-small cell lung cancer (NSCLC): Association between CT-based imaging features and EGFR and K-RAS mutations in 122 patients—An external validation. European Journal of Radiology. 2019;110:148-155. https://doi.org/10.1016/j.ejrad.2018.11.032
- Rizzo S, Savoldi F, Rossi D, et al. Radiogenomics as association between non-invasive imaging features and molecular genomics of lung cancer. Annals of Translational Medicine. 2018;6(23):447. https://doi.org/10.21037/atm.2018.11.17
- Rizzo S, Botta F, Raimondi S, et al. Radiomics: the facts and the challenges of image analysis. European Radiology Experimental. 2018;2(1):36. https://doi.org/10.1186/s41747-018-0068-z
- Elhalawani H, Lin TA, Volpe S, et al. Machine Learning Applications in Head and Neck Radiation Oncology: Lessons From Open-Source Radiomics Challenges. Frontiers in Oncology. 2018;8:294. https://doi.org/10.3389/fonc.2018.00294
- De Jong EEC, van Elmpt W, Rizzo S, et al. Applicability of a prognostic CT-based radiomic signature model trained on stage I-III non-small cell lung cancer in stage IV non-small cell lung cancer. Lung Cancer. 2018;124:6-11. https://doi.org/10.1016/j.lungcan.2018.07.023
- Rizzo S, Botta F, Raimondi S, et al. Radiomics of high-grade serous ovarian cancer: association between quantitative CT features, residual tumour and disease progression within 12 months. European Radiology. 2018;28(11):4849-4859. https://doi.org/10.1007/s00330-018-5389-z
- Jethanandani A, Lin TA, Volpe S, et al. Exploring Applications of Radiomics in Magnetic Resonance Imaging of Head and Neck Cancer: A Systematic Review. Frontiers in Oncology. 2018;8:131. https://doi.org/10.3389/fonc.2018.00131
- Rizzo S, Petrella F, Buscarino V, et al. CT Radiogenomic Characterization of EGFR, K-RAS, and ALK Mutations in Non-Small Cell Lung Cancer. European Radiology. 2016;26(1):32-42. https://doi.org/10.1007/s00330-015-3814-0
- Volpe S, Mastroleo F, Krengli M, et al. Quo vadis Radiomics? Bibliometric analysis of 10-year Radiomics journey. Eur Radiol (2023). https://doi.org/10.1007/s00330-023-09645-6
See open positions related to radiomics and artificial intelligence in the "Work with Us" section.
Last update date: 21/07/2023













